The full version of this post originally appeared on Medium.
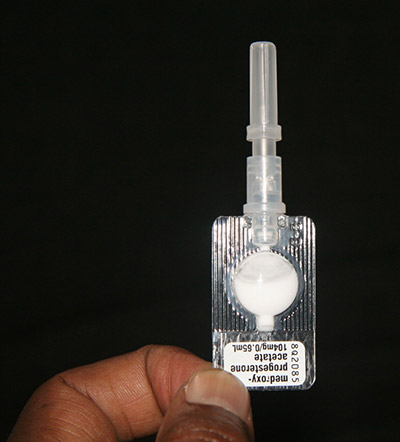 Self-management. Self-testing. Self-awareness. These are three pillars of self-care interventions that can help promote the sexual and reproductive health and rights (SRHR) of women, men and youth according to new guidelines released by the World Health Organization (WHO). WHO defines self-care as “the ability of individuals, families and communities to promote health, prevent disease, maintain health, and cope with illness and disability with or without the support of a healthcare provider.” Self-care as part of reproductive health is not a new concept. Throughout history, people have sought to control their fertility. However, in the context of a global shortage of trained health care workers and with an estimated 214 million women in developing countries who still have an unmet need for contraception, both new and existing SRHR self-care interventions can play a critical role in helping close the gap while at the same time empowering individuals to take control of their health.
Self-management. Self-testing. Self-awareness. These are three pillars of self-care interventions that can help promote the sexual and reproductive health and rights (SRHR) of women, men and youth according to new guidelines released by the World Health Organization (WHO). WHO defines self-care as “the ability of individuals, families and communities to promote health, prevent disease, maintain health, and cope with illness and disability with or without the support of a healthcare provider.” Self-care as part of reproductive health is not a new concept. Throughout history, people have sought to control their fertility. However, in the context of a global shortage of trained health care workers and with an estimated 214 million women in developing countries who still have an unmet need for contraception, both new and existing SRHR self-care interventions can play a critical role in helping close the gap while at the same time empowering individuals to take control of their health.
This July is self-care month, and FHI 360 is excited to join partners around the world in advancing strategies to meet the SRHR needs of women, men and youth through evidence-based self-care interventions. There are six ways that FHI 360 is helping advance the SRHR self-care agenda.
Read the complete post.

 Self-management. Self-testing. Self-awareness. These are three pillars of self-care interventions that can help promote the sexual and reproductive health and rights (SRHR) of women, men and youth according to
Self-management. Self-testing. Self-awareness. These are three pillars of self-care interventions that can help promote the sexual and reproductive health and rights (SRHR) of women, men and youth according to