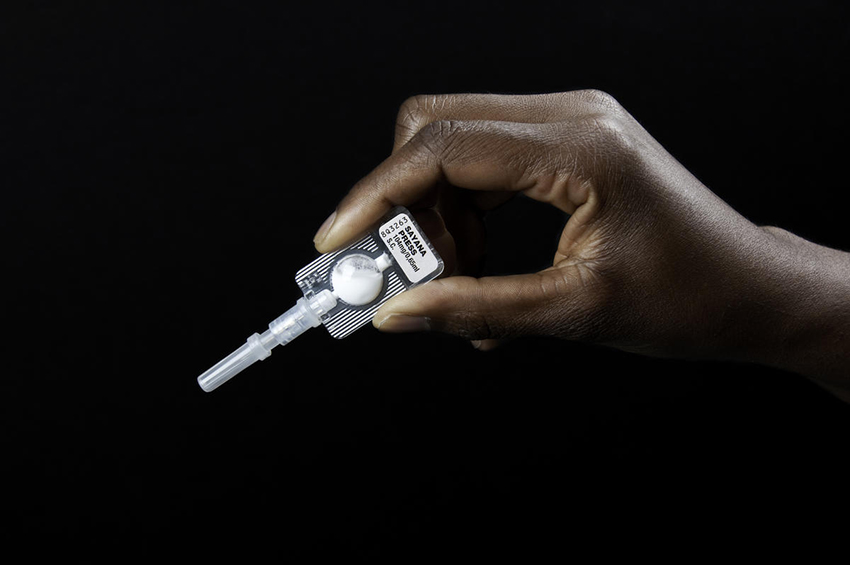
The injectable contraceptive, subcutaneous DMPA (DMPA-SC or brand name Sayana® Press) in the BD Uniject™ injection system. Photo: © 2012 PATH/Patrick McKern, Courtesy of Photoshare
Why do women who do not want to get pregnant choose not to use modern family planning methods? While this question is not bounded by geographies, the most recent Guttmacher Institute report, which focused on the low- and middle-income countries, is most illuminating. The two most common answers given by married women were health reasons/side effects or fear of side effects (26 percent) and claims of infrequent sex or not being sexually active (24 percent). Among unmarried women, infrequent sex (49 percent) was the top reason.
Equally informative are recent FHI 360 findings from a user preference study in Uganda and Burkina Faso showing that 75 percent of women currently using a method would be open to trying new technologies. It quickly becomes clear that existing methods do not satisfactorily address the changing needs of women throughout their 30- to 40-year reproductive journey.
Not to be forgotten, male contraceptive methods remain limited, even though acceptability research indicates that a substantial number of men would use family planning options themselves, if available.
What are we doing to address these concerns and to fill remaining gaps in the method mix? Clearly not enough … and clearly not fast enough! The truth is the contraceptive product development cycle is long (10-15 years or more), complex (with numerous clinical studies/trials required to prove safety and efficacy), and financed with fewer public and private investment dollars than most therapeutic areas.
These realities cannot deter us.
In the nearer term, we need to continue to refine existing products to improve their side effect profiles. For hormonal methods, the goal should be to hone in on the lowest doses required to ensure efficacy, while looking to extend duration of effectiveness and improve ease of use.
In the mid-term, we need to identify new delivery platforms that allow for self-administration — which will let potential users control their fertility discreetly and more conveniently, a preference noted by many in a recent study of Sayana® Press. In addition, we need nonhormonal methods for women who have sex infrequently and do not want a hormonal systemic approach. And, we need to develop new methods for men; having only two choices — the condom and vasectomy — leaves many men frustrated that they cannot be in more control of their own fertility.
In the longer term, we need transformational approaches. Just as the pill revolutionized birth control 60 years ago, the next generation of contraceptive technologies should aim to do the same. Like many other areas of medicine, future contraceptive technologies may shift from a one-size-fits-most approach to individualized solutions. Personalized contraception, perhaps informed by findings about the human genome, could minimize side effects while maximizing health benefits at the individual level.
At each step of the way, we need to listen carefully to what women and men want. I recently attended a workshop in India where participants from many walks of life spent time imagining the next generation of contraceptives, grounded in their own realities. The ideation exercises were challenging to us scientists in the room as we had switch our thinking from why novel ideas could not work — based on current physiology knowledge — to how we might make them work.
Over the next few months, K4Health and FHI 360 are focusing on contraceptive technology innovation. Our new Topic Page showcases key information, messages and resources on contraceptive research and development. As part of this thematic focus, our blog series will explore contraceptive technology innovation from three perspectives. First, several colleagues will discuss why we need to continue investing in this area and how future research needs to be framed. Next, a few contraceptive scientists will highlight some of the exciting work they are doing to move the field forward. Finally, key product introduction stakeholders will share insights on taking new methods over the finish line — commercializing them and scaling them up across the world. This last component is critical because, unless new products are acceptable, affordable and accessible to individuals in a variety of contexts, they will have minimal impact on method uptake and continuance.
As I approach my 35th anniversary in the field of contraceptive technology, I am still excited to be part of the movement to empower women and men to control their reproductive destinies. For all of those scientists who paved the way (like Dr. Richard Richter of Poland, who inserted the first IUD in 1909), for all the women and men who have participated in clinical trials in an effort to support the next contraceptive discovery, and for all the researchers and key stakeholders currently working in the field, this series is in tribute to you. Keep up this important fight; millions are depending on you!

Thank you.As a man and health provider i will educate and provide varieties of the already approved contraceptives.Looking forward to the expansion of male contraceptive.